HEALING THE NATION
Advancing Mental Health and
Addiction Policy
Where to Begin?
Health care in the United States is fractured and fragmented. Too often, mental health and addiction are treated separately from physical health, making it challenging for people to get timely access to quality mental health and addiction services. This framework provides federal policymakers with actionable solutions at each entry point — whether a specific population, access point, or intervention strategy — for comprehensive, inclusive mental health and addiction policies.
"
When healthy community conditions, good coverage, and inclusive policies are in place, we can achieve positive outcomes that improve the mental health and well-being of all Americans.
What is the
problem?
2018 marked the longest sustained decline in U.S. life expectancy since 1920. For the past three years, Americans have died younger and younger, primarily due to deaths from drugs, alcohol, and suicide. More lives were lost to these deaths of despair in 2017 than ever before.
While we have made tremendous innovations in health care, our health and well-being continues to suffer.
Why is this
happening?
Individual-level factors like loneliness, isolation, and a lack of belonging;
Systemic elements such as fragmented care delivery, lack of culturally effective care, and limited affordable access to care;
Social and community conditions like economic exclusion, housing and food insecurity, systemic racism and intergenerational trauma, and inequitable divisions of resources.
What are the
challenges?
- About 33% wait more than a week to access a mental health clinician
- Approximately 50% drive more than one hour round-trip to mental health treatment locations1
- 50% of counties had no psychiatrist in 2016
- 111 million people live in areas with mental health professional shortages2
- 10% with an identified substance use disorder (SUD) received care
- A mental health office visit with a therapist is five times as likely to be out-of-network when compared to a non-mental health office visit3
What are the solutions?
Policymakers at all levels have an opportunity to address these issues. To accomplish meaningful change, we must develop a comprehensive agenda with inclusive solutions.
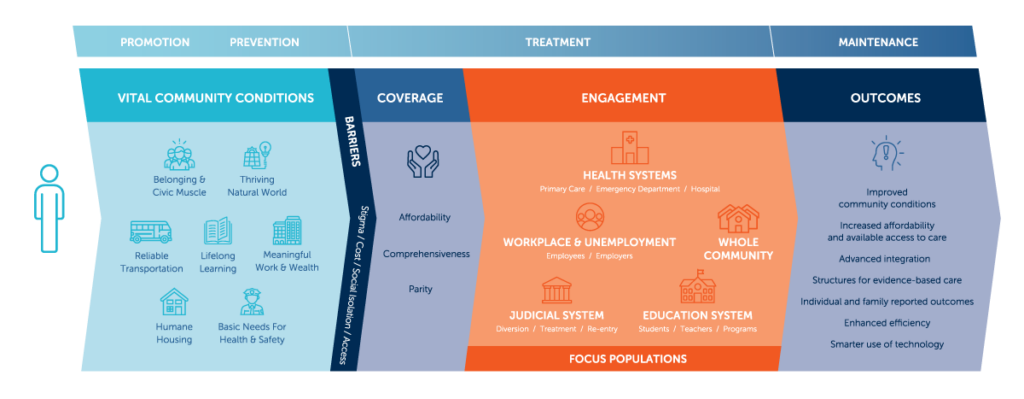
Framework for excellence in mental health and well-being
The framework for excellence in mental health is a guide for changemakers at every level of society who seek to improve mental health outcomes and promote well-being for millions of Americans.